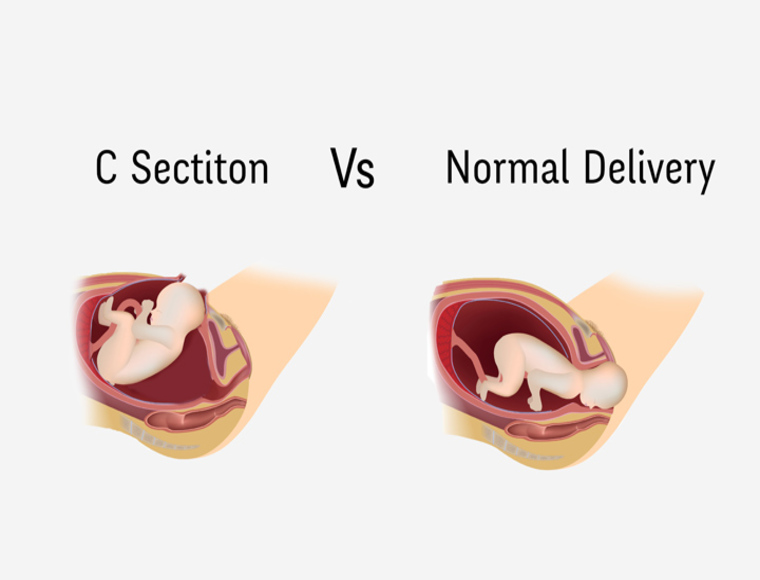
C-section vs. Normal delivery – How are they different?
As you near the delivery date, you should know in detail about the two childbirth procedures. Normal or vaginal delivery and cesarean delivery. Knowledge of the procedures will help you anticipate what happens when the time is due and help you deal with anxiety and fear.
There are possibly a lot of questions in your head such as ‘which delivery method would be safe for my baby,’ ‘is it going to be painful,’ or ‘how long would it take?’ and so on. Well, that’s normal, and you would be relieved once you see your baby.
Vaginal birth or Normal delivery
The stages of a vaginal birth
For women who deliver vaginally, childbirth progresses in three stages:
Stage 1: Labor
Labor itself is divided into three phases — early labor, active labor and transitional labor. All women who deliver vaginally will experience all three phases of labor, though you may not notice the first phase at all. The timing and intensity of contractions can help clue you in to which phase of labor you’re in, while periodic physical exams will confirm your progress.
Stage 2: Pushing and delivery of the baby
This is when your cervix reaches the magic 10 cm mark — meaning you’re fully dilated. Now it’s your turn to push your baby the rest of the way through the birth canal. Unless you’re laboring down (in which case you’ll catch a break for a few minutes to an hour while your uterus does most of the work bringing baby farther down into the birth canal).
You may wonder: Does pushing hurt more than contractions? Most women actually find that transitional labor, or those last 2 to 3 cm of dilation, is the most demanding and intense phase of labor. But it’s fortunately also the shortest, usually lasting 15 minutes to an hour. As your baby crowns and you push him or her out, you will feel a tingling, stretching or burning sensation (it’s called the “ring of fire” for a reason).
Stage 3: Delivery of the placenta
The worst is over. In this final stage of labor, you’ll continue to have mild contractions as your practitioner helps you deliver your baby’s placenta. He and she will examine it as well as your uterus to be sure everything’s as expected.
Will I Need Vaginal Stitches After Childbirth?
You may need vaginal stitches after childbirth if you experience vaginal tearing during birth. Even a little tear of the skin around the entrance to the vagina might require some stitches, while a more severe tear will definitely require stitches. Vaginal tears are more common for a first birth . They are also during a quicker birth where the vaginal tissue has had less time to stretch.
What Are The Benefits Of Vaginal Delivery?
For The Mother
- Mother and baby interaction:Women have expressed higher satisfaction, improved interaction with the baby, and control over the delivery in the case of vaginal delivery.
- Breastfeeding:Vaginal delivery also aids better maternal breastfeeding success through breast milk maturation. Skin-to-skin contact during normal delivery also leads to better outcomes with regards to breastfeeding and infant crying.
- Maternal mortality:Studies comparing maternal mortality between cesarean and normal delivery have shown that the risk is low in normal delivery than it is in c-section.
- Faster recovery:The recovery time after delivery is shorted with vaginal delivery than with cesarean delivery. It takes just one or two days to recover after a normal delivery, and about two weeks to resume the daily activities.
- No risks of surgery:There is no anesthesia given and no surgery done in the case of normal delivery. There won’t be any stitches or scars, and there is no need to worry about surgery-related risks such as infections, blood clots, hemorrhage, or reactions to anesthesia.
For The Baby
- Brain development:Yale School of Medicine’s research states that during vaginal birth, Ucp2 (a protein) is triggered in the hippocampus (a small brain organ), aiding the infant’s brain development. It also results in better neurobehavioral and physiological functions.
- Baby gets beneficial bacteria:During vaginal birth, the baby goes through the birth canal. Here, it gets exposed to bacteria that are known to be beneficial for its immune health, brain, and digestive health. It even helps in preventing infections.
- Low risks of TTN:Just before birth, the baby’s lungs are filled with fluid. When the fluid remains even after the birth, the baby may develop a condition called transient tachypnea of the newborn (TTN). However, with vaginal delivery, the fluid is cleared out while the baby is passing through the birth canal. Hence, there is almost no risk.
C-section
What happens during a cesarean section?
Whether it’s a scheduled surgery or a last-minute decision, the typical C-section is straightforward and follows a tightly-scripted game plan.
Preparation and anesthesia
A C-section begins with a routine IV and anesthesia — usually an epidural or spinal block, so the lower half of your body will be numb but you’ll stay awake. Then you’ll be prepped by having your abdomen shaved (if necessary) and washed with an antiseptic solution.
The operating room staff will insert a catheter into your bladder and place sterile drapes over your tummy. Your birthing coach or partner will be outfitted in sterile garb and allowed to sit near your head and hold your hand.
The emergency room staff will place a short screen blocking your vision of your abdomen, so the field remains sterile and so you don’t have to watch yourself getting cut. If you’re opting for a “gentle C-section”, the drape will be clear; otherwise, you can also ask for a mirror to watch. Even if you don’t want to see the cut, you will want to catch a glimpse of your baby as she emerges, so ask your practitioner to lift the little cutie up for a quick peek after delivery.
Incision and delivery
Once you’re either totally numb or fully asleep, the doctor will make a small incision in your lower abdomen — it may feel like your skin is being unzipped — just above your pubic hair line. With some neat suturing, the scar should be fairly unnoticeable and will fade more and more over time. Your doctor will then make another incision in the lower part of your uterus. For both incisions, two options are possible (and your two may not be the same):
- A low-transverse incision. This cut, across the lower part of the uterus, is used in 95 percent of C-sections. It is because the muscle at the bottom of the uterus is thinner (which results in less bleeding) and is also less likely to tear during subsequent vaginal deliveries.
- A vertical cut. This incision, down the middle of your uterus, is usually only required if the baby is nestled low in your uterus or in another unusual position.
Next, the amniotic fluid will be suctioned out and right after that your baby will be brought into the world (you might feel a bit of tugging). Because the excess mucus in her respiratory tract wasn’t squeezed out during a journey through the birth canal. Some extra suctioning will be necessary to clear those little lungs before you hear that first cry.
Meeting your baby
After the umbilical cord is cut, the surgeon will remove your placenta. They will then quickly do a routine check of your reproductive organs. Then you’ll be stitched up with absorbable stitches in your uterus (the kind that won’t later need to be removed). Either stitches or surgical staples on the abdominal incision. That procedure can take 30 minutes or longer.
You may receive antibiotics (to minimize your risk of infection) and oxytocin (to control bleeding and help contract the uterus) in your IV. Your blood pressure, pulse, rate of breathing and amount of bleeding will be checked regularly.
What Are The Benefits Of C-Section Delivery?
For The Mother
- Planned delivery: Usually, a cesarean is planned based on the health conditions of the mother and the baby. The doctors plan the entire procedure to bring the baby into the world safely. The procedure is mostly under control.
- No labor pain: As it is a surgical procedure, the mother does not go through labor or experience the pain that she otherwise would have in normal delivery.
- Reduced time: In recent years, the cesarean techniques have been simplified. The results are minimal loss of blood, shorter operating time, and higher patient satisfaction.
- Reduced risk of incontinence: There is no stretching or tearing of the vaginal with cesarean surgery. So there is a lower risk of pelvic prolapse, anal and urinary incontinence .
- Reduced risk of infection transmission: A few studies have found that there is no or reduced risk of transmission of hepatitis B virus. Or other infections to the infant with the elective cesarean procedure. This risk is high in the case of vaginal deliveries.
For The Baby
- Reduced trauma: As the baby doesn’t have to pass through the birth canal during a c-section procedure, there is no stress or trauma to the baby. The baby is directly and safely taken out of the mother’s womb.
- Reduced or no injury: There are fewer or almost no risks of injury to the baby through a cesarean delivery.
- Safe delivery with abnormal conditions: Sometimes, the baby settles down in the mother’s womb in certain abnormal positions (such as transverse lie or breech). Or the mom could have conditions like placenta previa (placenta covering the cervix). In such situations, vaginal delivery could be risky, and a c-section would ensure your baby is safe.
In the end, the best birth is the one that’s safest. Any delivery that brings a healthy baby into the world and into your arms is a perfect delivery. Talk to your doctor before you decide.